Hirschsprung's Disease
Hirschsprung's Disease, usually diagnosed in newborns, is a birth defect that affects about l out of 5,000 individuals. Those affected with this birth defect are missing intestinal nerve cells called ganglion cells. These nerve cells allow the intestine to relax so stool (poop) can pass through the intestine and out of the body. Without these nerve cells the intestine cannot relax and becomes very narrow. When the intestine is narrowed stool cannot easily pass. As a result, newborns with Hirschsprung's Disease often cannot have bowel movements on their own and have severe constipation.
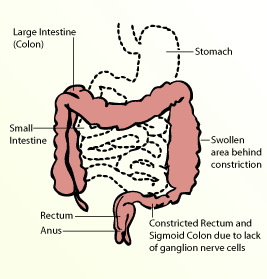
Usually Hirschsprung's disease affects only a small part of the large intestine/colon (near the rectum. Less commonly, in some individuals, all of the large intestine (colon) is missing ganglion cells. Very rarely, ganglion cells may be absent in both the large and small intestine.
How is Hirschsprung's Disease diagnosed?
Most newborns have a bowel movement in the first 1 to 2 days after birth. Hirschsprung's Disease is usually suspected when a baby does not have a bowel movement for several days following birth or has bowel movements infrequently. Babies with Hirschsprung's disease can have a large, swollen abdomen and may vomit green liquid after feeding.
There are two tests commonly used to make the diagnosis of Hirschsprung's Disease. The first is a contrast enema. During this test a liquid (contrast) fills the large intestine through a small tube placed into the anus (enema). X-ray pictures are taken as the liquid enters the intestine. If Hirschsprung's disease is present, the pictures of the intestine will show a wide (dilated) area followed by a narrow area of intestine. The narrow area is the part of the bowel without ganglion cells. The wide area of the intestine is healthy bowel filled with stool that cannot be passed.
The second study is a rectal biopsy where small samples are taken from inside of the large intestine, near the anus. This is done one of two ways. For infants, the pediatric surgeon removes two to three tiny pieces of intestine using a small suction device placed into the anus. This procedure is not painful and can be done as an office procedure without anesthesia. Older children will have the samples taken by the pediatric surgeon in the operating room, under anesthesia. Biopsy samples are examined under a microscope for the ganglion cells. If ganglion cells are seen in the biopsy samples, the intestine is normal and there is no Hirschsprung's Disease. If no ganglion cells are seen on the biopsy samples, the diagnosis of Hirschsprung's Disease is made. If these suction biopsy samples are not adequate for analysis the surgeon may need to take additional biopsy sample in the operating room under anesthesia.
Late diagnosis
While most babies are diagnosed very soon after birth, some children may not be suspected to have Hirschsprung's disease until much later in life. These children often have severe constipation, with formed stool above the narrow segment of the intestine with watery stools passing around it. They are also prone to slow weight gain. Those patients diagnosed later in life often need to undergo a staged repair with a temporary stoma as described below.
How is Hirschsprung's Disease treated?
The part of the intestine without ganglion cells must be removed with an operation. Usually, in newborns, this can be done in one operation (primary repair). In most babies we operate without making an large incision (surgical cut) on the abdomen. Most often, the surgeon will use laparoscopy (telescopes through the abdomen) in addition to operating through the anus to repair the Hirschsprung's disease.
In some babies more than one operation may be required. This is called a staged repair. In the first operation (or first stage), normal intestine is brought out as a temporary stoma, and the portion of the intestine without ganglion cells is bypassed.. A stoma is an opening on the abdomen where the intestine is brought out to the skin. If your child has a stoma, stool will drain into a pouch (bag) worn on the outside of the body. Several months later, the portion of the intestine without ganglion cells is removed and the intestine is sewn together in order to close the stoma. Your child's pediatric surgeon will talk to you about the best operation for your child.
In most Hirschsprung's operations, there is very little blood loss. You child will receive blood only in the rare case of an extreme emergency. If you wish to provide a directed donation of blood, contact our office, 2-3 weeks in advance of the operation.
After the operation, your child will have will have very frequent loose stools. It will be important to protect the skin around the anus at all times. The surgical nurse will recommend barrier pastes for the diaper area or teach you how to mix and apply a cream called "butt balm". Use this cream at all times to protect the skin from the irritating effects of diarrhea. The recipe for butt balm is: a four ounce tube of Desitin® ointment, a one ounce bottle of Stomahesive® powder combined to create a cream the consistency of peanut butter. Ilex cream can also be used to protect the skin against irritation from diarrhea. All of these products are available over the counter. If your child has a stoma, the same precautions will also be needed to protect the skin in the diaper area after the stoma is closed.
If your child has a stoma, the surgical nurse will teach you to apply the pouch and care for the stoma. Ostomy supplies will be ordered from a home care company to be delivered to your home.
How long will my child be in the hospital?
If your baby has transanal surgery without a stoma, he or she will go home in about one to three days. If your baby has a stoma, he or she may stay in the hospital longer. In either case, your baby will be ready to go home when he or she is having bowel movements, eating and drinking without vomiting, and is comfortable on pain medication taken by mouth. The surgical nurse specialist and your bedside nurse will ensure you trained and able to care for you child's stoma before discharge.
What is enterocolitis?
Enterocolitis is an inflammation of the intestine which can occur in children with Hirschsprung's even after their operation. Signs and symptoms of enterocolitis are abdominal swelling, vomiting and diarrhea, fever and lethargy. This disorder can be serious and can require hospital admission, IV fluids and electrolytes, antibiotics and colonic decompression with normal saline irrigation. Occasionally, severe cases can require another operation and can even be fatal if not treated.
Abdominal swelling without vomiting and diarrhea, fever, and lethargy can be managed with outpatient colonic irrigation with normal saline. This procedure will be taught to you in clinic by our nurse practitioner.
Homecare after surgery
If your baby has anal surgery, he or she will go home in about three days. Your baby will most likely have a lot of diarrhea, and it will be important to protect the skin around the anus at all times. Use the recommended paste constantly to protect the skin from the irritating effects of diarrhea.
If your baby has a stoma, he or she may stay in the hospital longer. The temporary stoma will remain in place for several months, and during that time stool will drain into a pouch worn on the outside of the body. Your child's nurse will teach you how to take care of the stoma and protect the skin from the irritating effects of the stool.
Pain Management
Prescription pain medication (narcotics) is not usually needed once your child is home. Most children only need Acetaminophen (Tylenol®) or Ibuprophen (Motrin®). Give the medication according to the dosage directions on the label. If your child is still uncomfortable call our office.
Care of Dressings
If your baby has an incision on the abdomen there will be a gauze pad and clear plastic dressing in place, this dressing is to be removed 2 days after the operation. Under this dressing will be pieces of tape called Steri-strips®. On the Steri-strips®, there may be a small amount of blood. This is normal. Your child can bathe with the Steri-strips® in place. These can be pulled off one week after the operation. The skin around the incision may be red and bruised and slightly swollen. This can last several weeks. There will be no visible stitches to remove because they are under the skin. The stitches will dissolve after several weeks. Sometimes these stitches are irritating and will come out of the skin, through the incision. If this happens the incision will look red and may drain white, yellow or red fluid. This can be normal for some children and will get better with time and daily bathing.
Care of Incisions
If your child has an incision, the wound is closed with dissolvable suture (stitches). These stitches are under the skin and do not have to be removed. In some children these stitches may poke through the skin about 4 weeks postoperatively. This may be associated with a little local redness and pus and it may involve an end of the incision or a larger portion. This is normal and is best treated by gently cleansing the area with soap and water and waiting. When the suture falls out or completely dissolves, the wound will heal. If your child has worsening redness, swelling pain of the incision and a fever within 2weeks of the operation, please call our office.
Healing Ridge
If your child has an abdominal incision, you will feel a firm ridge just under the incision once it is healed. This is called a healing ridge and it is normal to find after surgery. The healing ridge lasts for several months before it softens and disappears.
Bathing Restrictions
Your child may bathe (or shower) as soon as two days after surgery. Once your child is feeling better, before discharge or at home, he or she may bathe (or shower). Bathing is a good way to clean and soothe the anal area and gently clean the skin without injury. Some parents prefer to use a hair dryer, on the low (cool) setting, to dry the anal area well before putting on more protective cream. If your child has a stoma, the pouch can be removed and your child can be placed in the bath. This will not harm the stoma and is recommended.
Stoma Care
The pediatric surgery nurse specialist and bedside nurse will teach you to care for your child's stoma.
Skin care of diaper area
A diaper rash can occur rapidly and take days or weeks to heal. We recommend that you continuously apply the recommended protective skin care products. Begin as early as the day after surgery. Do not stop using the skin protective products until the number of bowel movements becomes less, usually after many weeks. If your child develops a rash that does not get better, please call our office. Here is a suggested routine.
- Remove all butt balm (see below) cream, paste or ointment daily with mineral oil applied gently with cotton balls.
- Soak your child's bottom in a tub of warm water after applying the mineral oil.
- Clean gently with soap and water, do not scrub skin. Avoid making the skin bleed.
- At the end of the bath, pat at the skin dry.
- Apply Cavilon 3 M No Sting Barrier Film by swab or spray to all affected skin in the diaper area.
- Let dry for 60 seconds
- Apply butt balm or other barrier paste over the 3 M product.
- After each bowel movement, clean the poop off the butt balm and do not rub the butt balm from the skin.
- Reapply the butt balm to the diaper area.
- Repeat after each bowel movement.
- Repeat mineral oil and bath each day.
Butt Balm Recipe
The recipe for butt balm is: a four ounce tube of Desitin® ointment, a one ounce bottle of Stomahesive® powder, mixed well. These products are available in stores or on-line. No prescription is needed.
Activity Restrictions
Your child can return to doing his or her usual activities without any special restrictions, unless the pediatric surgeon tells you otherwise. If your child is school age, school activities can begin again as soon as he or she feels well enough. If you need a letter sent to your child's school about the operation and recovery, please call our office. If your child has a stoma, supplies will be ordered for your baby. You will be taught how to take care of the stoma and use the supplies before going home.
Do I see the surgeon again after the operation?
If your child has a stoma, you will need to make an appointment to be seen one month after discharge. If your child has a primary surgery or stoma closure, he or she will need to be seen in the Pediatric Surgery office two weeks after the operation. At this visit, his or her anus will be checked to make sure the opening is large enough for stool to pass easily. Sometimes a child's anus has to be dilated, or stretched, for several weeks or months following surgery. If this is necessary, your child's surgeon or surgical nurse will teach you how to do dilations at home.
Why does my child need anal dilators?
You will receive a set of anal dilators before you leave the hospital. Bring these to your first surgical appointment. Some anal incisions heal by contracting and becoming tight. This is called a stricture. If this happens, passing bowel movements will be very difficult. Stretching the anal incision gently with anal dilators may be recommended by your child's pediatric surgeon. If your child's pediatric surgeon recommends the use of dilators at your first appointment, you will need to follow their instructions carefully. This is essential to prevent stricture. If you are having problems with anal dilation contact the surgical nurse practitioner.
When do I call the surgeon's office?
Call our office at 415-476-2538 for the following:
- Any concerns you have about your child's recovery
- A temperature of 101°F or higher
- A red incision
- Increasing pain and tenderness at the incision
- Any liquid coming out of the incision
- A change in the number of bowel movements each day
- No bowel movement for one day
- Foul smelling bowel movements
- Abdominal distention
- Vomiting
- Red rash around the anus that is not getting better
- Any questions concerning your child's stoma
Parent Support Organizations
Pull-Thru Network Inc.
http://www.pullthrough.org
2312 Savoy Street
Hoover, Alabama 35226-1528
205.978.2930
[email protected]
Colonic irrigation with normal saline for treatment of Hirschsprung's Enterocololitis
Introduction
The pediatric surgeon may recommend that your child undergo rectal irrigations to treat enterocolitis that can occur before or after surgery. Irrigations will clean the intestine of stool to prevent bacterial overgrowth, infection and treat diarrhea. Irrigations are usually started in the hospital and may need to be continued at home.
Supplies
- Silicone Foley catheter the size of your child's thumb (16 Fr. for children under one year of age to a maximum of 24 Fr. for children over one year of age). It may be necessary to put additional holes on the side of the catheter. The Foley balloon is NEVER inflated.
- DO NOT USE RED RUBBER CATHETERS. They are too stiff.
- A 60 ml catheter tip syringe.
- Normal Saline Solution
- 2 re-usable basins and a large plastic bucket.
- Water soluble lubricant (K-Y jelly or similar)
Giving the irrigation
- Pour normal saline solution into one of the basins
- Draw up 20 ml of saline into the 60 ml syringe
- Lubricate catheter and gently insert 6 inches into the anus.
- DO NOT INFLATE THE FOLEY BALLOON.
- The tip of the catheter is in the right place when there is a gush of air/liquid stool through the catheter.
- If air or stool drains from the catheter, attach the syringe to the end of the catheter and slowly push in the saline.
- Pull back on the plunger to allow the stool and saline to return. If there is no return flow, disconnect the syringe from the catheter and allow fluid to drip into the other basin. If return flow is slow, remove the catheter, clear the holes of stool and reinsert the catheter.
- If drainage is still inadequate, after the above measures, discontinue the procedure and contact the pediatric surgeon.
- If drainage is satisfactory, you may continue.
- Repeat the process, 20 ml at a time, making sure the volume of fluid drained is greater than or equal to the volume of being pushed in. By the time the clean basin is empty of normal saline solution, the soiled basin should be filled with an equivalent volume of stool and saline.
- Empty dirty basin into large plastic bucket and refill clean basin with normal saline. solution
- Continue irrigation until return flow is clear.
Irrigations are performed one to three times in a day, as instructed by the surgeon.
Recipe for normal saline solution
The safest saline solution to use is commercially prepared and purchased from a pharmacy. Saline solution can be made at home, but if mixed incorrectly using too much salt, it is dangerous and can cause seizures and coma.
If mixing at home follow this recipe exactly:
- 1 and ½ teaspoons salt
- 1 liter (or 1000 ml) tap water
- Stir until dissolved.
Anal dilations at home
Supplies
Gather dilator, K-Y lubricant, clean diaper, wipes and someone to help you, if needed.
Directions for anal dilations at home
- Position your child on his/her back, holding the feet toward the head with knees flexed.
- Lubricate the dilator and gently insert into the anus as instructed.
- A very small amount of bleeding may occur, this can be normal.
- Withdraw the dilator. Clean with soap and water.
- Continue the dilations, at home using starting dilator size as directed by surgeon.
- Use twice daily, for one week.
- Every week, change to a dilator that is one size larger.
- Use twice daily for one week.
- Stop increasing the size once you get to the maximum size as directed by your surgeon.
Tapering dilations
- Continue twice daily dilations for 2 weeks using dilator size as directed by surgeon.
- Decrease frequency to once daily for 2 weeks.
- Decrease to every Monday, Wednesday and Friday for 2 weeks.
- Decease to once a week for 2 weeks.
- Stop dilations.*
*Do not discard your dilators. They are to be cleaned with soap and water and saved in the event they need to be used again.
Regular follow up is recommended for bowel management of children with Imperforate Anus and Hirschsprung's Disease in our LIFE clinic.
